While companies have been very busy trying to keep up with all of the changes and new COVID-19 related legislation such as the expansion of FML regulations to include the Families First Coronavirus Response Act or FFCRA, OSHA has been busy investigating the huge influx of COVID related whistleblower complaints.
Out of those complaints, OSHA has issued over 200 citations and has proposed penalties totaling $2,856,533 solely for Coronavirus related violations. One quick glance at the list of citations and penalties issued, and it becomes very apparent that the key regulations being cited are those within the Respiratory Protection standards and include:
If you’re an employer who has handed out N-95 respirators to your workforce without providing fit testing, medical evaluations or specific training or if you’ve not implemented a written respiratory protection program to include the management of all of these things, you’re opening the door to being cited and fined as well as potentially aggravating pre-existing medical conditions like asthma and COPD.
In this article, we’ll provide you with a few general facts about personal protective equipment that you might not have known as well outline the three primary types of face coverings being used during the pandemic and how they fit into the respiratory protection standards.
Since the pandemic started, there has been quite a bit of discussion about personal protective equipment or “PPE” like gloves, gowns, face coverings and goggles to name a few different types. What we haven’t heard much about is the difference between their use by the general public and their use in the workplace and why those two things are different or about the requirements imposed on employers when deciding to incorporate PPE.
OSHA’s sole purpose is to ensure safe and healthy working conditions for workers in the United States mainly by setting and enforcing regulatory standards. The regulatory requirements OSHA develops and enforces are intended for the workplace only—not for the general public.
Why does this matter? It matters because most regulatory requirements set forth by OSHA don’t really translate to the general public. For example, the use of face coverings as a protection from COVID-19 has been hotly discussed on social media platforms and at times, OSHA’s stance on cloth face coverings has been included in that discussion. OSHA has indicated that cloth face coverings aren’t the best protection from COVID-19 transmission in the workplace and aren’t a substitute for surgical masks or N-95 respirators. The intent of this statement wasn’t to say that cloth face coverings don’t work, but rather to say that in workplaces where employees are exposed to hazards like COVID-19 on a routine and ongoing basis, that employers are responsible for providing adequate protection to their workers—and cloth face coverings generally aren’t going to do that.
The workplace environment where someone is going to be routinely exposed to hazards for the duration of a workday is quite a bit different than a member of the general public spending an hour in a grocery store or at a restaurant. So, the idea that OSHA says cloth face coverings aren’t adequate to protect workers from routine and constant exposures to airborne contaminants shouldn’t be taken to mean that cloth face coverings won’t protect you while you’re at Target shopping for housewares.
In addition to all of this, companies should understand that prior to arbitrarily requiring certain PPE to be used in the workplace, employers are first required to assess the work environment for hazards, like those from airborne contaminants (among many other hazards). If hazards are discovered, it may seem like putting everyone in PPE is the simplest way to protect workers—but that’s not how things work.
When workplace hazards are discovered, OSHA prohibits employers from skipping past trying to reduce or eliminate those hazards through engineering and/or administrative controls and going right to PPE as a form of protection. What this means is that if a workplace hazard is discovered, an employer can’t simply put everyone into PPE without first attempting to eliminate the hazard through other means—like engineering or administrative controls. In fact, OSHA states very clearly that PPE should always be used as a last resort because it is the least effective means of protection.
In the case of COVID-19 exposure, the employer is still required to determine the potential for exposure and based on that, should look for ways of engineering out or administratively controlling the exposure first. If engineering or administrative controls won’t sufficiently reduce the exposure or aren’t feasible, PPE can be used to supplement those efforts. Here’s an example of how this might work.
Example: A company has employees working in close contact with one another in a part of the building where the ventilation system (HVAC) is not functional. After determining that workers have a potential exposure hazard to COVID-19 from working so closely together, the hierarchy for reducing or eliminating that hazard should look like this:
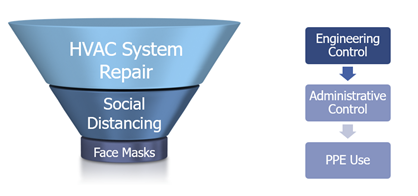
In this example, the employer would work on getting the HVAC system repaired to provide adequate ventilation. If the HVAC system can be repaired but is found to be too old to adequately provide sufficient ventilation to the workers, the employer should still have it repaired but would also want to provide additional means of protection, such as the social distancing of workers or maybe reducing the number of workers allowed to work in that area, etc. In both cases, the employer can and should consider adding PPE to help further reduce the exposure however, the employer cannot simply ignore the first two steps and go straight to PPE use as a sole means of protection.
OSHA does things this way for a reason. By requiring employers to assess their workplaces for specific hazards, they are forcing employers to identify unsafe workplace conditions—and then do something about them. In addition, by having the hierarchy of controls in place for eliminating or reducing hazards, it forces employers to do their best to try and eliminate or reduce hazards instead of automatically going to PPE which is often the least expensive and least effective means of protection.
When PPE is going to be used to supplement other controls or in cases where it’s simply not possible to implement engineering or administrative controls and PPE is going to be required, with a very few exceptions, employers are required to provide these items to their workforce free of charge. They are also required to provide training on any required PPE that must include things like how to use it, how to care for it and what limitations there are with its use. If PPE is going to be optional, employers can choose whether they want to allow employees to use their own personal PPE in the workplace or not.
Now that we’ve discussed PPE and understand that an employer cannot simply put employees into PPE without attempting to implement engineering or administrative controls first and that employers are responsible for providing most required PPE to their workers free of charge, let’s talk about the Respiratory Protection standard.
Considering that COVID-19 is a respiratory virus which is thought to be somewhat contained by the use of face coverings or face masks, it should come as no surprise that a good number of the citations OSHA has issued during the pandemic are violations of the Respiratory Protection standard.
Knowing what we know about COVID-19, the natural instinct for many employers has been to simply provide face masks to their workforces or require workers to provide their own respiratory protection—but it’s not that simple. Within the Respiratory Protection standards are very specific regulations about the use of respiratory protection in the workplace—and some of them may surprise you. For example, that box of N-95 masks (often called dust masks or filtering facepieces) that you purchased at Home Depot or on Amazon for your employees are actually considered respirators by OSHA and they come with a series of regulatory requirements which we will discuss later in this article.
In addition to N-95 masks, during the COVID-19 pandemic, we’ve seen two other types of face coverings being used and talked about. To make things a bit less confusing, we’re going to provide a deeper explanation of the three most commonly used face coverings and how they each fit into the Respiratory Protection standards.
Let’s start this discussion by talking about cloth face coverings. These are the type of face coverings you see many people wearing out in public. They can be purchased online and in most stores and can also be made at home using things like t-shirts, bandanas and other fabrics.
If you’ve worn a cloth face covering like this, then you’re aware that they are generally loose fitting and don’t provide a good seal to the face. Because they also generally don’t include a filter and/or aren’t made from material designed to act as a filter, they should be considered more of a temporary barrier for those times when protection is needed while at the grocery store or while standing in line somewhere. However, they are not adequate to provide a sufficient level of protection to workers who are going to be exposed to airborne contaminants routinely during the workday or where respirators are required. Because of this, cloth face coverings are not considered to be a form of PPE and cannot be used as an alternative to surgical masks or where respirators like N-95 masks are required to protect workers from airborne hazards in the workplace.
Because of this, cloth face coverings are not included in the Respiratory Protection standards. This doesn’t mean that employers can’t allow their employees to wear them, it just means that in environments where airborne hazards exist, like those from COVID-19, the employer cannot allow cloth face coverings to be used as a form of protection. These face coverings are perfectly acceptable to allow employees to wear if the work environment doesn’t present a known exposure to airborne contaminants or other particulate hazards and if an employee wants to wear one just because it makes them feel more comfortable.
Unlike cloth face coverings, surgical masks are typically cleared or approved by the U.S. Food and Drug Administration (FDA) and can be comfortably used by most people without issue. When worn properly, surgical masks can provide some protection against splashes and sprays from things like sneezes and coughs with the primary benefit however, being to contain the wearer’s own respiratory emissions (droplets). For example when a surgeon wears a surgical mask to prevent contaminating surgical sites or when a dentist or hygienist wears a surgical mask to protect patients during treatment. In both of these examples, the surgical mask is being worn to contain the wearer’s respiratory droplets, rather than being used as protection from someone else’s sneezes and coughs.
Because surgical masks provide this benefit, OSHA does consider them to be personal protective equipment (PPE) and includes some regulatory requirements such as training to make sure workers are aware of their limitations and to show the wearer how to use and care for them.
While surgical masks are a step up from cloth face coverings, they do have similar limitations in that they are also loose fitting, don’t provide a good seal to the face and don’t include a filtration element which makes them inappropriate in environments where respirators are required. As a result, surgical masks cannot serve as an alternative to respirators like N-95 masks.
There are a good number of different types of masks that fall into this category however, the most commonly used type are N-95 masks. For a mask to be considered a “filtering facepiece”, it must be certified by the National Institute for Occupational Safety and Health (NIOSH) as being constructed of materials that are proven to filter a specific amount of particulate. For example, an N-95 mask will filter out 95% of particulates like dust and/or airborne diseases like COVID-19.
Masks in this category are considered to be respirators by OSHA which gives them a somewhat substantial place within the Respiratory Protection standards. Because they are included in the standards, they are regulated just like other more complex respirators and require fit testing, a medical evaluation and specific training among other things. OSHA has published a few temporary enforcement waivers on some of these requirements however, in general these things are all still required to be complied with.
For employees who are choosing to voluntarily wear an N-95 mask in places where their use is not required, they need to be given training and must also be given an Appendix D document which outlines pertinent information about their use.
So, if you went out to Home Depot and bought a box of N-95 masks and told your workers to wear them without making sure they were fit tested, medically evaluated to ensure they didn’t have a medical condition that would prohibit their use (like asthma or COPD) and if you didn’t provide any training on their limitations, how to wear them and how to care for them—you’re going to need to do that. And, in addition to these things, you’ll need to create a simple respiratory protection program that includes all of this information and how you’re going to manage this program.
To find several valuable resources about how to develop and manage these things, check out OSHA’s COVID-19 page, dedicated to all things COVID-19 related. This page is updated frequently and includes several excellent resources as well as all of the information on how OSHA expects companies to manage things during the pandemic.
Once you’ve developed your written program and have made sure your workers are properly fit tested, evaluated and trained, managing these things doesn’t have to be complicated if you’re using EHS Insight! With our Health Encounter and Training Management modules, you can manage the respirator fit tests and medical evaluations as well as ensuring training is being conducted timely.
Contact us to find out more!
Katy Lyden is a Domain Analyst and EHS Subject Matter Expert for StarTex Software, the company behind EHS Insight. Prior to her current role, Katy spent 17 years successfully leading EHS programs for several large companies within the manufacturing industry. Katy is a Navy veteran, retired Emergency Medical...